Does BMI matter for orthopedic outcomes? Recent studies suggests that the adverse surgery outcomes associated with BMI are not as severe as previously thought. As such, orthopedic physicians are re-evaluating the practice of denying their patients surgery on the basis of BMI alone.
However, beyond surgery outcomes, BMI still matters. In fact, it’s often what brings a patient to the operating table in the first place. Orthopedic physicians should, as always, carefully evaluate new evidence and incorporate it into their existing treatment paradigm to maximize patient outcomes and promote overall patient wellness.
BMI and Orthopedic Surgery Outcomes
Recent evidence suggests that a high BMI should not be the deciding contraindication for orthopedic surgery. For example, one study found that, although there is an association between BMI and total knee replacement outcomes, the association is not significant enough to warrant surgical restrictions on the basis of BMI alone.
Likewise, perspectives among orthopedic physicians are shifting to accommodate this evidence, along with a higher prevalence of obesity among their patient populations. To illustrate, as many as 55% of patients presenting to total joint arthroplasty clinics are obese.
Why Weight Loss for Orthopedics?
The correlation between obesity and MSK health means that operating on obese patients is increasingly unavoidable. However, while it may be the case that obesity will not severely compromise surgery outcomes, BMI still matters. Here’s why:
- Obese individuals are 20 times more likely to require total knee replacement surgery than non-obese patients.
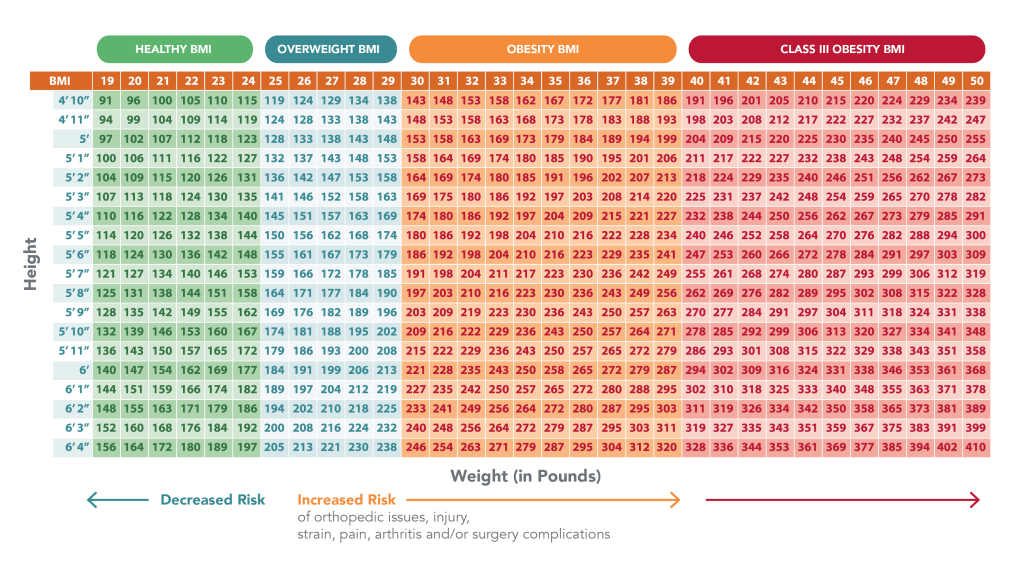
- The odds of sustaining an MSK injury are 15% greater for overweight individuals and 48% greater for individuals with Class III obesity.
- Every 1 pound of excess weight causes an added 4 pounds of pressure on the knee joint and 10 pounds of pressure on the lower back.
In sum, excess weight can both cause and exacerbate MSK injury and disease. In fact, a high BMI is often what brings a patient to the operating table in the first place. Yet obesity is a highly preventable risk factor.
Using the ratios above, a patient who loses just 10 pounds of body weight can alleviate 40 pounds of pressure on their knee joint and 100 pounds of pressure on their lower back, preventing a significant amount of “wear and tear” on their joints over time.
Leveraging Conservative Treatments
While it may be the case that operating on patients with a high BMI carries less risk than previously thought, there is a consensus among orthopedic surgeons that conservative treatment options—including physical therapy and weight loss—should be exhausted before recommending surgery to patients.
Unfortunately, according to an article published in Arthroscopy, Sports Medicine, and Rehabilitation, “…there is a documented lack of implementing an appropriate course of conservative care, especially physical therapy, prior to surgery across multiple orthopedic disciplines including sports, spine, and trauma medicine and joint arthroplasty.”
While orthopedic surgeons care greatly about maximizing their patients’ outcomes, including helping them avoid surgery, many outside factors prevent them from the practical application of conservative treatments. These include time restraints, out-of-pocket costs for patients, expectations regarding non-surgical treatments versus surgery, and communication barriers, to name a few.
There are several promising approaches to overcoming these obstacles. First, orthopedic surgeons can collaborate with their non-surgical care team to create a standardized strategy that adequately documents conservative treatment outcomes to inform surgical decision making.
With the increased availability of Telehealth and remote monitoring solutions, orthopedic surgeons can alleviate time and cost pressures that prohibit them from implementing this more extensive approach to treatment.
An evidence-based remote monitoring program such as Prescribe FIT, for example, assures that patients receive high-value conservative orthopedic treatment to decrease weight, reduce pain, and improve mobility without significant cost to the practice or increased workload for staff.
Conclusion
Does BMI still matter for orthopedic outcomes? While evidence suggests that patients should not be denied orthopedic surgery on the basis of BMI alone, there remains a significant opportunity to help maximize patients’ MSK health via weight loss for orthopedics, rather than proceeding directly to surgical intervention.
Likewise, remote patient monitoring technologies can help streamline the implementation of these treatments, allowing orthopedic surgeons to overcome the obstacles preventing them from taking a more proactive approach towards their patients’ health.
For more information about Prescribe FIT, visit https://www.prescribefit.com/practices/.
Published on February 27, 2023

